If you\’ve ever experienced the persistent heel pain associated with plantar fasciitis, you\’re not alone. This common foot condition can disrupt your daily life and mobility, but the good news is that help and relief are within reach. At Paul Miller Podiatry, we understand the challenges that plantar fasciitis presents and are here to guide you through understanding and managing this condition effectively.
Plantar fasciitis is a topic that affects many individuals, and in this blog post, we\’ll provide you with valuable insights into the causes, symptoms, diagnosis, and the range of treatment options available. Whether you\’re seeking ways to alleviate your discomfort or exploring preventive measures, this guide will equip you with the knowledge you need to take control of your foot health. Let\’s embark on a journey to understand and manage plantar fasciitis for lasting relief and improved well-being.
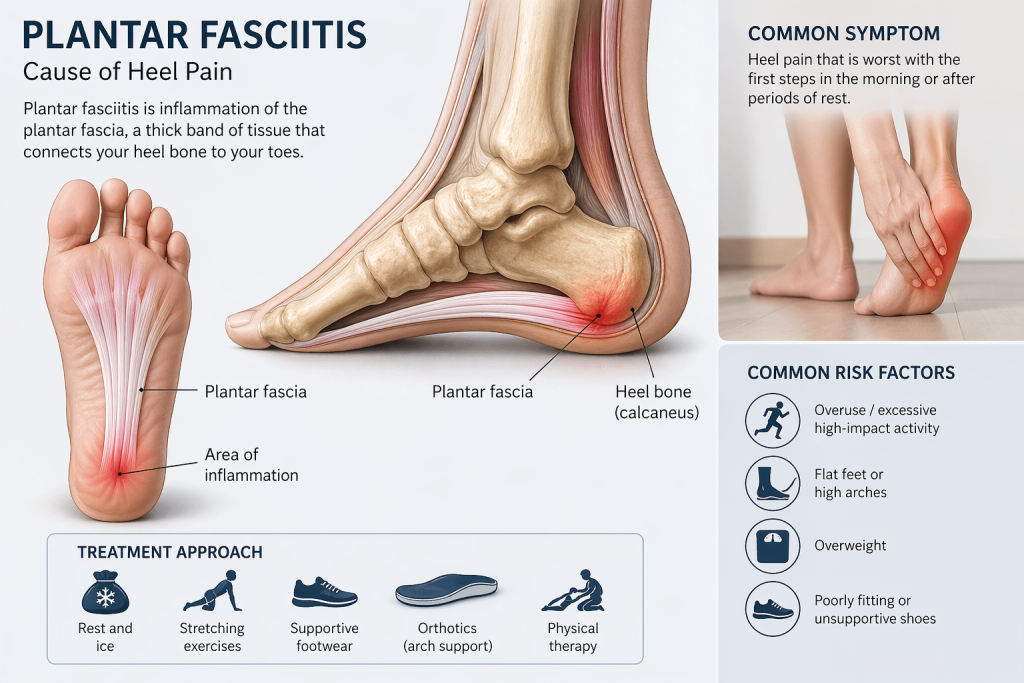
What Is Plantar Fasciitis?
Plantar fasciitis is a common and often painful foot condition that affects the plantar fascia, a thick band of tissue running along the bottom of your foot, connecting your heel to your toes. This condition typically develops when the plantar fascia becomes inflamed or experiences micro-tears, leading to pain, especially in the heel area.
The primary role of the plantar fascia is to support the arch of your foot and absorb the shock generated during walking, running, and other activities. When it\’s strained or injured, it can result in discomfort, stiffness, and sharp pain, particularly during the first steps in the morning or after prolonged periods of rest.
Plantar fasciitis can be caused by various factors, including overuse, improper footwear, high-impact activities, and underlying foot mechanics. Understanding the causes and symptoms of plantar fasciitis is the first step in effectively managing this condition and finding relief. In the sections that follow, we\’ll delve deeper into the risk factors, recognizing symptoms, and treatment options for plantar fasciitis.
Common Risk Factors
Several factors can increase the risk of developing plantar fasciitis. Understanding these risk factors can help you take preventive measures and reduce your chances of experiencing this painful condition. Here are some of the most common risk factors to be aware of:
1. Age:
Plantar fasciitis is more prevalent in individuals between the ages of 40 and 60. As we age, the plantar fascia can naturally lose elasticity and become more susceptible to injury.
2. Foot Mechanics:
Certain foot mechanics, such as having flat feet or high arches, can alter the distribution of weight and pressure on the feet, increasing the risk of strain on the plantar fascia.
3. Activity Level:
Engaging in high-impact activities like running, dancing, or sports that involve repetitive foot movement can put stress on the plantar fascia, increasing the risk of injury.
4. Improper Footwear:
Wearing shoes with inadequate arch support or improper cushioning can lead to poor shock absorption, placing additional strain on the plantar fascia.
5. Obesity:
Carrying excess body weight can add extra stress to the plantar fascia, as well as the muscles and ligaments that support the feet, raising the risk of injury.
6. Occupations:
Certain occupations that require prolonged periods of standing or walking on hard surfaces can contribute to plantar fasciitis.
7. Rapid Changes in Activity:
Abruptly increasing the intensity or duration of physical activities can strain the plantar fascia, making it more susceptible to injury.
8. Tight Calf Muscles:
Having tight calf muscles can affect your gait and foot mechanics, potentially leading to plantar fasciitis.
Understanding these risk factors can help you make informed choices to reduce your likelihood of developing plantar fasciitis. Whether you\’re looking to prevent this condition or seeking relief from existing symptoms, knowledge of these risk factors is a valuable tool in managing your foot health effectively.
Recognising Symptoms of plantar fasciitis
To effectively manage and address plantar fasciitis, it\’s essential to recognize the common symptoms associated with this condition. By identifying these signs early, you can take the necessary steps to seek treatment and relief. Here are the typical symptoms of plantar fasciitis to be aware of:
1. Heel Pain: The hallmark symptom of plantar fasciitis is often sharp or stabbing pain in the heel, typically at the bottom of the heel or just in front of it. This pain is most noticeable with the first steps in the morning or after periods of rest.
2. Foot Arch Discomfort: Many individuals with plantar fasciitis experience aching or discomfort in the arch of the affected foot. This discomfort can extend along the length of the plantar fascia.
3. Pain After Activity: Pain tends to intensify during or following activities that involve weight-bearing on the feet, such as walking, running, or standing for extended periods.
4. Stiffness in the Morning: It\’s common for individuals with plantar fasciitis to feel stiffness in their feet, particularly in the morning. This stiffness often eases as you move and the tissues stretch.
5. Pain After Sitting: After sitting for a while, such as during work or extended periods of inactivity, you may experience an increase in heel pain when you stand up and start walking.
6. Increased Pain on Stairs: Climbing stairs or walking on uneven terrain can exacerbate plantar fasciitis pain due to the increased pressure on the heel and arch.
Recognizing these symptoms is the first step in addressing plantar fasciitis. If you or someone you know is experiencing these signs, seeking professional evaluation and treatment, such as consultation with a podiatrist, is crucial. Early intervention can lead to more effective pain relief and a quicker return to a pain-free, active lifestyle.
Treatment Options for plantar fasciitis
When it comes to managing plantar fasciitis, there are several treatment options available to alleviate pain, promote healing, and improve foot function. The choice of treatment often depends on the severity of the condition, individual preferences, and the guidance of a healthcare professional. Here are some common treatment options for plantar fasciitis:
1. Rest and Activity Modification:
One of the first steps in managing plantar fasciitis is to rest and reduce activities that exacerbate the condition. Avoid high-impact activities, and opt for low-impact exercises like swimming or cycling.
2. Ice and Anti-Inflammatory Medications:
Applying ice to the affected area can help reduce inflammation and relieve pain. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended by a healthcare provider for additional relief.
3. Stretching Exercises:
Regular stretching exercises that focus on the calf muscles, Achilles tendon, and the plantar fascia can improve flexibility and reduce tension in these areas.
4. Orthotic Inserts and Arch Support:
Custom-made or over-the-counter orthotic inserts and arch supports can provide better foot alignment, cushioning, and support, reducing stress on the plantar fascia.
5. Night Splints:
Wearing night splints helps maintain the foot in a dorsiflexed position overnight, stretching the plantar fascia and reducing morning pain.
6. Physical Therapy:
Physical therapy can offer tailored exercises and techniques to strengthen the foot and calf muscles, improve flexibility, and promote proper gait.
7. Corticosteroid Injections:
In some cases, corticosteroid injections may be recommended to reduce inflammation and pain. These injections are typically administered by a healthcare provider.
8. Shockwave Therapy:
Extracorporeal shockwave therapy (ESWT) is a non-invasive treatment that uses sound waves to stimulate healing and reduce pain in the affected area.
9. Bracing and Taping:
Braces and taping techniques can provide additional support to the foot, reducing tension on the plantar fascia.
10. Medical Interventions: – In severe or persistent cases, medical interventions such as platelet-rich plasma (PRP) therapy or surgery may be considered.
The most effective treatment plan for plantar fasciitis often involves a combination of these options. It\’s important to consult a podiatrist or healthcare professional to determine the best approach for your specific situation. Early intervention and a comprehensive treatment plan can lead to significant pain relief and a return to an active, pain-free lifestyle.
Footwear Choices, Orthotics, Exercises, Physical Therapy, Night Splints, and Bracing
Managing plantar fasciitis often involves a combination of strategies, and many individuals find relief through specific choices and interventions. Let\’s explore these effective approaches in more detail:
1. Footwear Choices:
Selecting the right footwear is a fundamental step in managing plantar fasciitis. Look for shoes with excellent arch support and cushioning to reduce strain on the plantar fascia. High-quality, supportive shoes provide comfort and stability, making them an essential component of your foot care routine.
2. Orthotic Inserts and Arch Support:
Orthotic inserts and arch supports are designed to improve foot alignment and cushioning. These devices can be customized to your specific needs or purchased as over-the-counter solutions. Orthotics work to reduce pressure on the plantar fascia and provide support during daily activities.
3. Stretching Exercises:
Regular stretching exercises can significantly benefit individuals with plantar fasciitis. Focus on stretching the calf muscles, Achilles tendon, and the plantar fascia itself. These exercises help to increase flexibility and reduce tension in these critical areas. Incorporate them into your daily routine for ongoing relief.
4. Physical Therapy:
Physical therapy is an invaluable resource for individuals with plantar fasciitis. Working with a physical therapist allows you to access personalized exercises and techniques that enhance foot strength, flexibility, and proper gait. A tailored physical therapy program can contribute to long-term pain reduction and improved mobility.
5. Night Splints:
Night splints are designed to maintain your foot in a dorsiflexed position while you sleep. This gentle stretching of the plantar fascia during the night can help alleviate morning pain and stiffness. Night splints are an effective way to promote healing and reduce discomfort.
6. Bracing:
Braces and taping techniques can provide additional support to your foot, particularly the arch and heel. These supportive measures work to reduce tension on the plantar fascia, offering relief during daily activities.
Incorporating these approaches into your daily routine can significantly enhance your ability to manage and find relief from plantar fasciitis. It\’s important to consult with a healthcare professional, such as a podiatrist or physical therapist, for guidance on implementing these strategies effectively. By combining these interventions with other treatment options, you can improve your chances of a successful recovery and a pain-free, active lifestyle.
Prevention of plantar fasciitis
Preventing plantar fasciitis is a proactive approach to maintaining healthy feet and avoiding the discomfort associated with this condition. Whether you\’ve experienced plantar fasciitis in the past or wish to reduce your risk of developing it, implementing preventive measures can make a significant difference. Here are some key strategies to consider:
1. Proper Footwear:
Invest in high-quality shoes with good arch support and cushioning. Replace worn-out shoes regularly, as worn-out footwear can lead to poor foot mechanics and increased strain on the plantar fascia.
2. Gradual Activity Changes:
If you\’re planning to increase your physical activity or change your exercise routine, do so gradually. Sudden, intense activities can strain the plantar fascia. Gradual changes allow your body to adapt to new demands.
3. Stretching and Warm-Up:
Prior to physical activity, perform proper stretching and warm-up exercises to prepare your muscles and tendons. Focus on stretching the calf muscles, Achilles tendon, and the plantar fascia.
4. Appropriate Surface:
When engaging in high-impact activities like running or jogging, choose surfaces that offer good shock absorption. Running on softer surfaces can reduce the impact on your feet.
5. Maintain a Healthy Weight:
Maintain a healthy weight to reduce excess pressure on your feet. Losing excess weight can alleviate stress on the plantar fascia and improve overall foot health.
6. Supportive Footwear:
If you have specific foot mechanics, such as flat feet or high arches, consider using orthotic inserts or arch supports to provide better foot alignment and support.
7. Stretching Routine:
Regularly perform stretching exercises for your calf muscles and the plantar fascia. These stretches can help maintain flexibility and reduce the risk of injury.
8. Listen to Your Body:
Pay attention to any signs of discomfort or pain in your feet. If you experience symptoms of plantar fasciitis, such as heel pain, consult a healthcare professional promptly.
9. Quality Footwear for Specific Activities:
Choose footwear designed for specific activities. For example, use running shoes for running and walking shoes for walking. This ensures that your shoes provide the right support for the activities you enjoy.
By incorporating these preventive measures into your daily life, you can reduce the likelihood of developing plantar fasciitis and maintain overall foot health. If you have concerns about your foot health or experience any discomfort, consulting with a podiatrist or healthcare professional can provide personalized guidance and recommendations. Prevention is a key to keeping your feet healthy, pain-free, and active.
Plantar Fasciitis help in Kent
Plantar fasciitis may be a common foot ailment, but it doesn\’t have to be a persistent source of discomfort. With a comprehensive understanding of the condition and a range of effective strategies at your disposal, relief is within reach.
At Paul Miller Podiatry, we\’re dedicated to helping you on your journey to healthier, pain-free feet. From understanding the causes and symptoms of plantar fasciitis to exploring various treatment options and prevention strategies, we\’ve equipped you with the knowledge to take control of your foot health.
Remember, early intervention and a proactive approach to managing plantar fasciitis are key to finding relief and maintaining an active, pain-free lifestyle. If you\’re experiencing symptoms or seeking guidance on plantar fasciitis, our team of experienced podiatrists is here to help. Don\’t hesitate to get in touch with Paul Miller Podiatry for personalized care and support.
Your feet are your foundation for daily life, and they deserve the best care. Reach out to us today and take the first step towards a future with healthier, pain-free feet.

